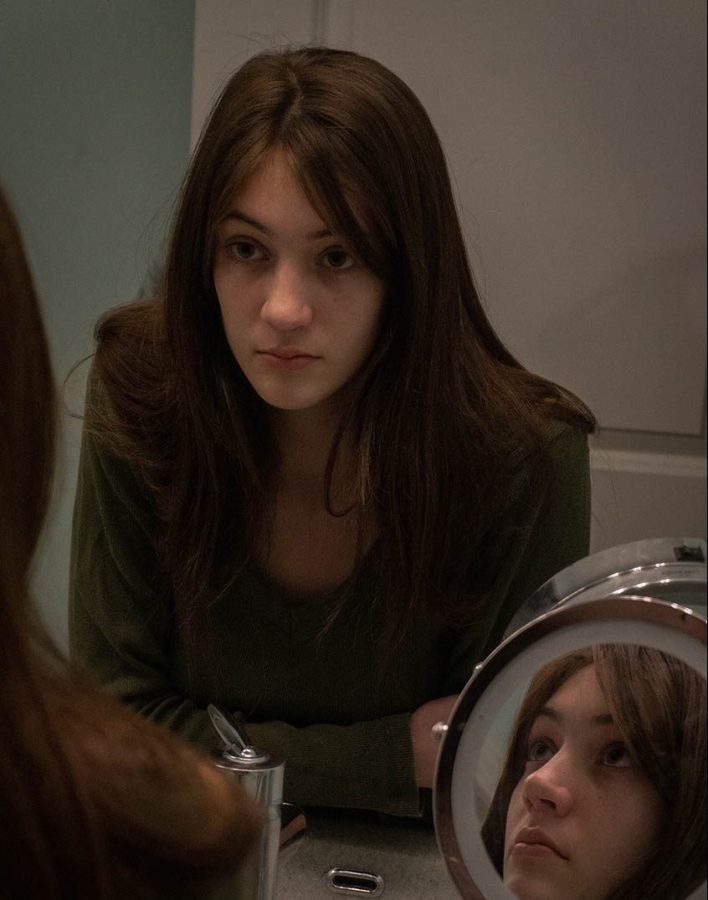Modern Medicine

Patients suffer from misdiagnoses
As sophomore Anna Wright was growing up, her dad began to worry about her. Although she seemed healthy, she had stopped gaining weight and growing taller.
“I fell off my growth curve, and I was a lot shorter than everyone else, so [my dad] started asking my primary care doctor about it. He would bring it up, and he researched it, and the doctors were always like, ‘No, it’s not a big deal. She’s fine. She’s just shorter,’” Wright said. “And they said it was nothing to worry about, so we kind of put it off for a really long time.”
Trusting her doctor’s advice, Wright tried to live her life as normally as possible. However, it was difficult as she watched her peers grow; she herself remained short until her parents took her to a specialist.
The endocrinologist ordered a growth hormone stimulation test. Wright took drugs to stimulate the production of growth hormone and then doctors drew her blood to see how much growth hormone she was producing.
“I wasn’t producing hardly any [growth hormone].That’s when [the doctors] knew there was a problem, and I’d have to start injections,” Wright said. “My pituitary gland doesn’t produce growth hormone on its own. Once you have one gland that isn’t producing a certain hormone properly, then it kind of messes with the rest of your hormones too, so I had blood sugar problems and a lot of other problems with my glands.”
According to a National Patient Safety Foundation survey, Wright’s experience mimics that of nine percent of people who report their doctors have failed to make an accurate diagnosis for them.
However, because of the high number of patients many doctors see daily, Timothy Fete, M.D., said small misdiagnoses are fairly common and insignificant.
“In primary care offices, where you’re seeing a child with a runny nose and a cough, you can miss a diagnosis. [You can] say that it’s a general cold and it’s really due to an allergy, but it wouldn’t have much impact on the child downstream,” Fete said. “If a doctor says a child doesn’t have appendicitis and a child does, then the child can get dramatically sicker. Medicine [is] not … an exact science, and a lot is based on following clues. All physicians misdiagnose some small percentage of patients they see.”
Misdiagnoses are also common because many unusual problems have different causes but end up producing the same final symptom, Fete said. For example, an infant who is fussy and seems gassy could have many problems: a food allergy, an anatomical problem, colic or an inability of the body to break down food. Although they are all very different conditions, they manifest in the same way.
“The doctor’s job is to try to take the most complete history of what’s going on with the patient and to do the best physical exam and pull that information together to come up with the most likely cause or a list of the most likely two or three causes of a particular complaint,” Fete said. “Generally the bottom line [is] anything a patient has as a concern can have a number of potential causes, so we have to do our best to find out what the true cause is with the history of what’s going on and with the physical exam and the least possible expensive exam to try and clench the diagnosis.”
The National Patient Safety Foundation survey found 42 percent of people to have had a misdiagnosis or treatment error. This was the case for senior Nicole Montgomery. In constant pain from swollen joints, she went to urgent care, only for the doctors to give her the wrong treatment.
Not getting better “made me really worried because I didn’t know if they were ever going to find out what was wrong with me,” Montgomery said. “I didn’t know what was going to happen.”
Concerned, Montgomery went to a rheumatologist. The doctor finally found she had a drug-induced lupus, an autoimmune disease where the body attacks its own immune system and causes swelling of the joints and severe arthritis. Going through the experience was not a positive time for Montgomery.
“I still trust [doctors], but it makes me think twice now and consider my own knowledge about my sicknesses. Like if I feel like I have a cold and they say I have cancer, I’m not going to believe them,” Montgomery said. “Luckily, even though they gave me a couple of prescriptions, it wasn’t terribly expensive for us to pay for.”
In both Montgomery’s and Wright’s cases, a specialist narrowed down a diagnosis; Fete recommends getting a second opinion to prevent misdiagnoses. Not only was it a relief for Wright to get better, but she also was happy to have the knowledge of what was wrong with her.
“It was really good to finally have diagnosis, and there was hope for me to get taller and that I wasn’t going to be short forever,” Wright said. “But it was also kind of aggravating to know that we could have known a lot sooner had the doctors listened to my parent’s concerns better.”
Living her life with uncertainty, however, had a lasting effect on Wright. Although she has one of her illnesses figured out and, because of the growth hormone shots, is now an average height, Wright battles reoccurring sinus infections and is currently recovering from her second round of mononucleosis. Because her original illness was not caught quickly, she struggles with not blowing these other problems out of proportion.
“If you think something’s wrong with you, don’t take no for an answer,” Wright said. “Listen to your gut. I mean, don’t be overly pushy because doctors usually know what they’re talking about, but you also kind of have to listen to your body and make your own calls about whether or not you think something’s not right.”
By Kirsten Buchanan
Long term illnesses plague teenagers
While junior Rachel Bryan’s friends skated around the roller rink, the number on her blood-testing meter was increasing exponentially. Despite Bryan’s attempt to keep her blood sugar at a normal level through insulin shots, the pump did not stop rising. In the middle of the roller rink birthday party, Bryan passed out.
“I kept re-checking my blood sugar, but it kept getting higher,” Bryan said. “I eventually passed out and woke up in the [emergency room] with a nurse standing above me saying, ‘Yay, she’s awake’. I found out my meter was malfunctioning, and I really had low-blood sugar.”
The roller-rink incident is just one of many setbacks Bryan has dealt with since being diagnosed with Type 1 diabetes at age seven. Although unrelated to her diabetes, Bryan also has a condition called aquagenic uritcaria where her skin will break out in hives if exposed to water for longer than 10 minutes.
“My older brother’s friend thought it would be funny to chase me around with a cup of sugar-water one time,” Bryan said. “The water because of my allergy and the sugar because of my diabetes; It was funny, and they didn’t mean anything by it, but then it got on me and it wasn’t very funny anymore.”
With both conditions, Bryan does not get to experience things the same way her friends do. She often feels different from everyone else because of the precautions she must take.
“I can’t just go places like my friends’ houses without bringing my diabetic supplies,” Bryan said. “I can’t just have a girl’s day and eat ice cream and cookie dough like everyone else without having high blood sugar.”
Similar to Bryan, senior Corbin Schleider discovered his disease from difficulties he had in day-to-day life. Prior to visiting a doctor, Shleider researched his seizures, finding out that he had generalized epilepsy.
“I had a few seizures and didn’t know what to think, so I decided to get tested,” Schleider said. “I’d looked into it and that’s the main reason I decided to go. They did an [electroencephalograph] and found out I had abnormal brain waves.”
Schleider’s condition starts out with myoclonic jerks, similar to twitches, then leads to a blackout. Schleider then has a seizure that can last up to five minutes. After the seizure hits, he is unconscious for around 20 minutes. Despite taking medicine to control his epilepsy, Schleider cannot stop the seizures once they start.
“I’ve had myoclonic jerks happen to me at school before but never a full tonic clonic seizure,” Schleider said. “I did have one at my friends house though. It was funny for me because when I woke up from it, my friends were freaking out and thought I was going to die or something.”
Schleider has found that a stable support system is the key to successfully managing his disease. When sophomore Eli Stout was diagnosed with Graves disease, an illness that attacks his immune system, he looked to his relatives for help and support through the tough time.
“My family’s response was worry and scared,” Stout said, “because Graves is an auto-immune disease; they didn’t like the idea of my body fighting against itself.”
Having a supportive family did not help Stout’s initial reaction. The doctor’s first believed Stout had post-concussion syndrome from football but then discovered both his pulse and blood pressure to be high.
Because of his illnesses, Stout had to undergo radioactive treatment. His reaction to the treatment caused him to have rhabdomyolysis, a breakdown of muscle fibers. High levels of creatine kinase enzymes, which help muscles function, led to a shutdown in his kidneys and liver for nearly three months.
“The biggest thing for me was realizing I wouldn’t be able to play football anymore because I could have just dropped over on the field,” Stout said. “But the worst part is all the blood work I have to get down and feeling tired and exhausted all the time. I realize that I’ll have to deal with it forever but it’s not that big of a deal anymore.”
With all chronic illnesses, support from family and friends helps ease the difficulty. Research assistant to Vicki Conn, Ph.D., Natalie Markis at University of Missouri—Columbia agrees that any routine, especially that of diabetes can get tiresome.
“I think the most challenging aspect of diabetes is self-management for a newly diagnosed patient [in the] modification of their diet,” Markis said. “The entire diabetic routine can lead to the patient [burning] out so having a good support system is key.”
With solid backing from friends and family, Bryan finds positives in her diabetes. Because of having to manage her blood sugar, Bryan is able to perform math problems more quickly and accurately.
While Bryan’s disease helps her in school, Schleider’s epilepsy has changed his view on life and helps him remain optimistic.
“Because I have it now I feel like I can relate to so many more people,” Schleider said. “I’m way more understanding of people who have diseases that aren’t necessarily cancer. I have a story to tell now about what I’ve been through and what I’m still going through. I think having it has made me such a better person.”
By Maddie Davis